TENS Therapy for Pain Relief: How Transcutaneous Electrical Nerve Stimulation Works and When It Helps
 Mar, 19 2026
Mar, 19 2026
When you’re stuck with chronic back pain, arthritis, or a flare-up of sciatica, reaching for another pill isn’t always the best move. Many people are turning to TENS therapy - a simple, drug-free way to ease pain using a small device that sends gentle electrical pulses through your skin. It’s not magic, but for a lot of people, it works. And unlike painkillers, there’s no drowsiness, no risk of addiction, and no stomach upset. The question is: does it work for you? And if so, how do you use it right?
How TENS Therapy Actually Stops Pain
TENS stands for Transcutaneous Electrical Nerve Stimulation. That’s a mouthful, but here’s what it really means: electrodes (small sticky pads) are placed on your skin near the area hurting, and a tiny device sends mild electrical pulses through them. These pulses don’t shock you - they tickle, buzz, or tingle. And that feeling? That’s the key.
Back in 1965, scientists Ronald Melzack and Patrick Wall came up with the Gate Control Theory. They figured your nerves work like a gate. When pain signals try to get to your brain, they get blocked if other signals - like touch or vibration - come in first. TENS uses electrical pulses to flood your nerves with those non-pain signals. It’s like turning up the volume on a song so you don’t hear the noise outside.
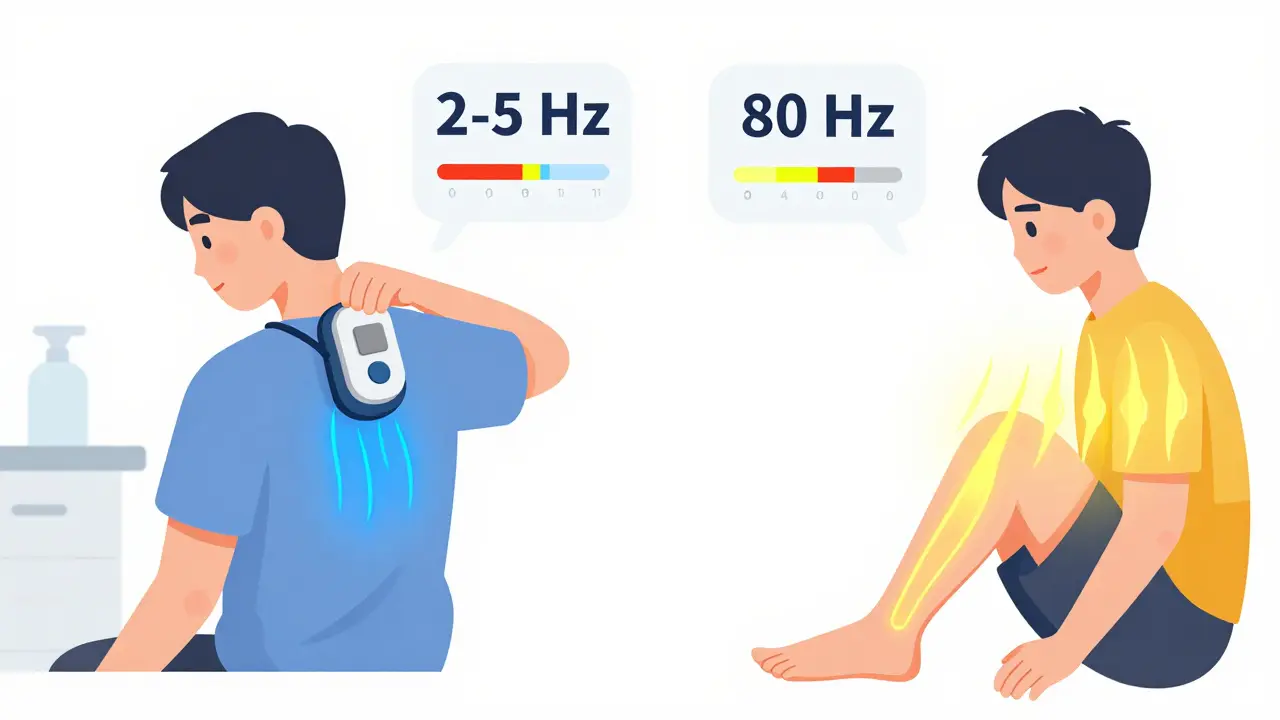
There’s another trick too. At low frequencies (2-5 Hz), TENS can trigger your body to release natural painkillers - endorphins. These are the same chemicals your brain makes when you run or laugh. That’s why some people feel relief that lasts even after the device is turned off.
Types of TENS Settings and What They Do
Not all TENS units are the same. Most have different modes, and picking the right one matters.
- Conventional TENS (50-100 Hz): This is the most common setting. It gives you a strong tingling sensation without pain. Best for acute pain - like after surgery or a sprained ankle. Works fast, but the relief usually stops when you turn it off.
- Low-frequency or Acupuncture-like TENS (2-5 Hz): Slower pulses, higher intensity. Feels more like a deep throb. Triggers endorphin release. Used for chronic pain like osteoarthritis or lower back pain. Relief can last hours after use.
- Burst Mode: A mix of the two. Pulses come in groups of 100 Hz, 2-3 times per second. Good for people who need both immediate and longer-lasting relief.
- Intense TENS: High intensity that causes a sharp, brief sensation. Used for only 5-15 minutes at a time. Helps by distracting the nervous system - kind of like slapping your knee when you stub your toe.
Most modern devices let you adjust intensity (0-80 mA), frequency (1-150 Hz), and pulse width (10-500 microseconds). The rule? Set it so you feel a strong, clear tingling - not painful, not faint. If you can barely feel it, it’s not working.
What Conditions Does TENS Actually Help With?
Research shows TENS works best for some things - and not so well for others.
- Strong evidence: Post-surgical pain, labor pain, osteoarthritis (especially knee), and acute muscle strains. A 2020 Cochrane review found TENS reduced labor pain by 31% compared to placebo.
- Moderate evidence: Chronic low back pain. A 2022 guideline from the American Physical Therapy Association says TENS gives about 15-20% more pain relief than fake devices - but results vary a lot from person to person.
- Weak or no evidence: Fibromyalgia, widespread nerve pain, or migraines. Only about 38% of fibromyalgia patients get real relief.
One study found TENS reduced opioid use by 27% after surgery. That’s huge. With the opioid crisis still ongoing, non-drug options like this are becoming more important. The CDC now recommends TENS as a first-line treatment for chronic pain - before pills.
Why TENS Fails for So Many People
Here’s the hard truth: TENS doesn’t work for everyone. And a lot of people give up too soon - not because it doesn’t work, but because they used it wrong.
Studies show that 68% of failed TENS treatments happen because the intensity was too low. If it feels like a gentle buzz, you’re not getting enough. You need to crank it up until the tingling is strong and clear - even if it’s a little uncomfortable. That’s the sweet spot.
Electrode placement is just as important. Put them too far from the pain, and the signal won’t reach the right nerves. For lower back pain, place them on either side of the spine, just above the hips. For knee pain, put one above and one below the kneecap. Most consumer units come with basic diagrams - but they’re often too vague.
Another big issue? Skin contact. If the electrodes dry out or shift during movement, the signal breaks. Using conductive gel can improve contact by 63%, according to electrotherapy experts. And if your battery dies after 90 minutes at full power? That’s normal. Most units last 8-10 hours on low settings, but high intensity drains them fast.
What Real Users Say
On forums like Reddit and WebMD, TENS gets mixed reviews - but the pattern is clear.
Positive users say things like: “I used to take two painkillers a day. Now I use TENS and barely need one.” Or: “It saved my workday after a long shift on my feet.”
Those who hate it? Usually because:
- The pads irritate their skin (34% complain on Drugs.com)
- The relief is inconsistent (29% on Reddit say they have to reposition electrodes every 10 minutes)
- They didn’t set it high enough (27% say they just didn’t know how to use it)
One user on Reddit, u/BackPainWarrior, summed it up: “TENS works great for my sciatica - but only if I crank it to 85%. Anything less just tickles. And yeah, the battery dies in 90 minutes.”
That’s the key: you have to experiment. What works for someone else might not work for you.
What to Look for in a TENS Device
There are hundreds of TENS units on the market. Here’s what actually matters:
- Adjustable intensity: Must go up to at least 70 mA. Cheaper units cap out at 30-40 mA - too weak.
- Multiple modes: At least conventional, low-frequency, and burst. Avoid single-mode units.
- Dual channels: Lets you treat two areas at once - like both knees or both sides of the back.
- Pre-programmed settings: Good for beginners. Look for presets labeled “back pain,” “knee arthritis,” etc.
- Rechargeable battery: Avoid units with disposable batteries. You’ll use it often.
- Clear instructions: Professional-grade units (like Omron Max Power) come with 140+ page manuals. Consumer units? Often just 8 pages. If it’s confusing, it’s not worth it.
Top brands: Omron, Chattanooga, and TechCare. Omron holds about a third of the market. Newer models now connect to apps via Bluetooth, letting you save your settings and track pain over time.
Who Shouldn’t Use TENS
TENS is safe for most people - but not everyone.
Avoid it if you:
- Have a pacemaker or implanted defibrillator
- Are pregnant (especially on the abdomen or lower back)
- Have epilepsy or a history of seizures
- Have open wounds or skin infections where the pads go
- Are using opioid medications - low-frequency TENS may not work as well because it competes with the drugs for the same brain receptors
If you’re unsure, talk to your doctor or physical therapist. Most clinics offer free trials.

Getting Started: What to Do First
Don’t just buy a unit and hope for the best. Here’s a simple 5-step plan:
- Identify your pain area. Is it localized (like a sore knee) or spread out (like lower back)?
- Choose a unit with adjustable settings and dual channels.
- Place electrodes within 2-3 cm of the pain, or over the nerve path. For sciatica, try the lower back and back of the thigh.
- Start with conventional mode (80 Hz). Increase intensity slowly until you feel a strong, steady buzz - not pain.
- Use it for 20-30 minutes, 2-3 times a day. Track your pain level before and after. Do this for 7 days.
If you don’t feel better after a week, try low-frequency mode. If that doesn’t work, talk to a physical therapist. They can show you exact placements and help you adjust settings.
The Future of TENS
TENS isn’t stuck in the 1980s. In May 2023, the FDA cleared the first AI-powered TENS device - NeuroLoop AI. It uses sensors to read your body’s response and adjusts the pulses in real time. Early trials showed 44% more pain relief than regular TENS.
Researchers are also testing “smart electrodes” with built-in sensors that monitor skin contact and automatically boost the signal if it weakens. The NIH just funded $2.4 million to develop them.
By 2025, experts predict TENS will be a standard part of digital health apps - syncing with your phone, tracking pain patterns, and suggesting when to use it. With opioid prescriptions falling and non-drug options rising, TENS isn’t going away. It’s getting smarter.
Frequently Asked Questions
Can I use TENS while sleeping?
No. You should never use TENS while sleeping. You won’t be able to adjust the intensity if it becomes uncomfortable, and there’s a risk of skin irritation or burns. Always use it while awake and alert.
How long does it take for TENS to work?
For most people, pain relief starts within minutes - especially with conventional mode. If you’re using low-frequency mode for endorphin release, you might feel the full effect after 20-30 minutes. Some people report lasting relief for hours after use.
Is TENS covered by insurance?
In the U.S., Medicare and many private insurers cover TENS units under code E0720 if prescribed by a doctor for specific conditions like chronic low back pain or post-surgical pain. Reimbursement is around $150. Check with your provider - you’ll usually need a prescription and documentation of failed conservative treatments.
Can I use TENS with other pain treatments?
Yes. TENS works well alongside physical therapy, heat packs, and even light exercise. It’s often part of a multimodal plan. But avoid combining it with other electrical therapies like IFC or NMES unless directed by a professional. Don’t use it while taking opioid painkillers if you’re using low-frequency mode - it may reduce effectiveness.
Do I need a prescription to buy a TENS unit?
No. You can buy TENS units over the counter without a prescription. But if you want insurance to cover it, you’ll need a doctor’s prescription. Also, if you have a serious medical condition, it’s wise to get professional advice before starting.

Allison Priole
March 21, 2026 AT 10:08I've been using TENS for my lower back pain for like 3 years now and honestly? It's been a game changer. I used to rely on ibuprofen like it was water, but now I barely take anything. The key is cranking it up-most people give up because it feels like a mosquito buzzing, but you gotta push it until it's that deep, kinda electric hum. Not painful, just intense. I use the burst mode, 20 mins twice a day, and it lets me sleep without waking up in agony. Also, gel pads? Life saver. I buy the conductive ones from Amazon, like $12 for 20. The device doesn't have to be fancy-mine's a $40 TechCare from Walmart and it still works like a charm.
Casey Tenney
March 22, 2026 AT 09:07This is why America is falling apart. People want magic solutions instead of doing physical therapy or lifting weights. TENS is a bandaid. A fancy, expensive bandaid. If your back hurts, strengthen your core. Do deadlifts. Stop being lazy.
Sandy Wells
March 23, 2026 AT 11:15TENS is overhyped. I tried it. Didn't work. My physical therapist said it's placebo for 70% of users. The rest just get lucky with placement. Also batteries die too fast. Why not just get a massage?
Bryan Woody
March 23, 2026 AT 19:57Oh wow look at this beautifully researched article full of citations and real data. How refreshing in a world of snake oil sellers. You know what's funny? The 68% of people who fail TENS? They're the same ones who set it to 'mild relaxation vibe' and then blame the device. I've seen people cry because it 'didn't work' when they were using 12 mA on a unit that goes to 80. Buddy, if you can't feel it through your jeans, you're not trying. Also, the AI-powered NeuroLoop? That's the future. We're talking real-time neuromodulation synced to your breathing. This isn't 1998 anymore. Stop using your grandma's TENS unit with duct tape holding the electrodes on.
Chris Dwyer
March 24, 2026 AT 10:41Hey if you're new to TENS and feeling discouraged-don't quit. I was skeptical too. I tried it for 3 days and gave up. Then I watched a PT video on YouTube-she showed exactly where to put the pads for sciatica (L4-L5 area + back of thigh) and I cranked it to 75. Felt like my leg was humming. 15 minutes later? Pain was 70% gone. Now I use it every morning before work. It's not a cure, but it's a tool. Treat it like a gym session-you gotta do it right to get results. And yeah, the battery dies fast, but I keep a power bank in my bag. Small price for freedom from pain meds.
Timothy Olcott
March 26, 2026 AT 03:59USA 4 LIFE 🇺🇸 TENS is why we beat China in innovation. Those commie countries don't even have real TENS units. My Omron lasted 5 years. No pills. No surgery. Just pure American engineering. 💪🔥
Desiree LaPointe
March 26, 2026 AT 21:22How quaint. A 1965 theory still being touted like it's gospel. Melzack and Wall were brilliant, yes, but we now know gate control is just one piece of a neuroplastic puzzle. And endorphins? Please. The placebo effect in TENS studies is 40% higher than in antidepressant trials. You're not 'releasing natural painkillers'-you're just feeling better because you spent $120 on a gadget and now you believe in it. Also, 'conductive gel'? That's not science, that's a marketing ploy from the 80s. I use saline-soaked cotton pads. Same effect. Cheaper. More sustainable.
Jackie Tucker
March 27, 2026 AT 18:00It's ironic, really. We've built a $2 billion industry around stimulating nerves with electricity to avoid the existential discomfort of being human. We've outsourced pain management to a battery-powered box because we're too afraid to sit with our suffering. TENS doesn't heal-it distracts. And distraction is the opiate of the modern age. The real question isn't whether it works-it's why we've come to need it so desperately. 🤔
trudale hampton
March 27, 2026 AT 19:55I love how this post breaks down the modes. I use low-frequency for my knee arthritis and honestly, the after-effect lasts like 4 hours. I didn't know that until I read this. Also, I never realized the battery drain was normal. Mine dies after an hour on high. Now I just charge it overnight. One tip: if you're using it on your back, try putting one pad high and one low-not side to side. It changes everything. Thanks for the detailed guide.
Shaun Wakashige
March 29, 2026 AT 03:13lol i tried it once and it just tickled. gave up. too much effort
Paul Cuccurullo
March 30, 2026 AT 04:03I appreciate the thoroughness of this piece. As a physical therapist, I recommend TENS to nearly every patient with chronic musculoskeletal pain-not as a cure, but as a component of a broader strategy. The real issue isn't the device-it's the lack of education. Most patients don't understand intensity, placement, or duration. We need more clinics offering 15-minute demos. The technology is there. The knowledge gap is what's failing people.